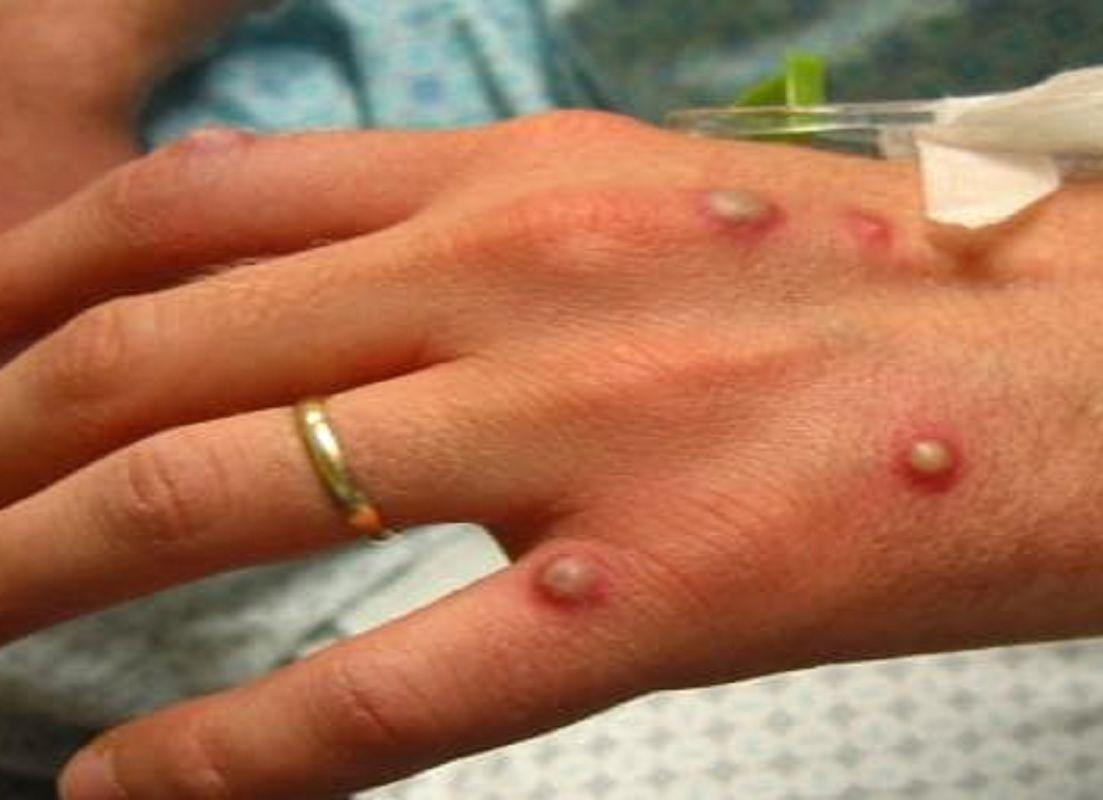
The Union Ministry of Health and Family Welfare verified the first monkeypox case in India on Thursday, with a tourist from the United Arab Emirates (UAE) who landed in Kerala three days ago testing positive for the viral illness. In response to a confirmed case of monkeypox in Kerala’s Kollam district, the Union Health Ministry dispatched a high-level multi-disciplinary team to work with state health authorities in implementing public health measures.
The Central delegation visiting Kerala included specialists from the National Centre for Disease Control (NCDC), Dr RML Hospital in New Delhi, top officials from the Ministry of Health and Family Welfare, and experts from Kerala’s Regional Office of Health and Family Welfare.
The team will collaborate closely with the state health departments to assess the situation on the ground and identify required public health initiatives. According to the Ministry of Health, the Centre is taking proactive measures by closely monitoring the situation and collaborating with states in the event of an epidemic.
“No need to panic as the centre has given fresh directions to all the states and Union Territories regarding monkeypox. It spreads through close contact with lesions, body fluids, prolonged contact with Respiratory Droplets and contaminated materials such as bedding,” official sources told ANI.
Kerala Health Minister Veena George said, “A Monkeypox positive case has been reported. He is a traveller from UAE. He reached the state on July 12. He reached Trivandrum airport and all the steps are being taken as per the guidelines issued by WHO and ICMR.”
Meanwhile, the Centre issued a letter to all states and union territories on Thursday, emphasising some of the critical activities needed to halt the spread of the illness.
Rajesh Bhushan, the health secretary, referenced a letter written by the government on May 31 in which it published thorough ‘Guidelines for Management of Monkeypox Disease.’
The health secretary directed all states and union territories to take key actions such as orienting and re-orienting all key stakeholders, including health screening teams at points of entry (PoEs), disease surveillance teams, and doctors working in hospitals, on common signs and symptoms, differential diagnosis, case definitions for suspect/probable/confirmed cases and contacts, contact tracing, and other surveillance activities that must be carried out.
He further requested that all suspect cases be screened and tested at entry points and in the community.
“Patient isolation (until all lesions have resolved and scabs have completely fallen off), protection of ulcers, symptomatic and supportive therapies, continued monitoring and timely treatment of complications remain the key measures to prevent mortality,” he said.
Bhushan stated that intensive risk communication directed at healthcare workers, identified sites in health facilities (such as skin, paediatric OPDs, immunisation clinics, intervention sites identified by NACO, etc.) as well as the general public about simple preventive strategies and the importance of timely reporting of cases must be implemented.
Hospitals must be identified, and appropriate human resource and logistical assistance must be provided to hospitals that are prepared to manage suspected/confirmed cases of monkeypox.
Also Read: India supplied over 235 million total supplies of COVID-19 vaccines to 98 countries: NITI Aayog VC
Monkeypox
Monkeypox, according to the World Health Organization (WHO), is a viral zoonosis (a virus transferred to people from animals) with symptoms comparable to those observed in smallpox patients in the past, however it is clinically less severe.
Monkeypox is spread to people by direct contact with an infected person or animal, or through contact with virus-contaminated material. According to the WHO, it is often a self-limiting condition with symptoms lasting two to four weeks.
The monkeypox virus spreads by intimate contact with lesions, bodily fluids, respiratory droplets, and infected items such as bedding.
According to WHO, a total of 3,413 laboratory confirmed cases of Monkeypox and one death have been reported to WHO from 50 countries/territories between January 1, 2022 and June 22, 2022.
The bulk of these instances (86%) have been recorded from Europe and the Americas (11 per cent).
This alludes to a modest but steady increase in the global dissemination of cases. Given that this is the first time that cases and clusters have been recorded concurrently in five WHO Regions, WHO has classified the worldwide risk of case spread as “Moderate.”