Bad Cholesterol: Bad cholesterol can be dangerous for many organs in the body, especially the heart and blood vessels. In this video, we will explain which organ is most affected by bad cholesterol and how you can effectively lower its levels. Take care of your health and learn simple ways to control bad cholesterol.”
Bad Cholesterol: A Silent Threat to Your Health
Cholesterol is a vital substance in our body, helping to build cells, produce hormones, and generate vitamin D. However, not all cholesterol is beneficial. There are two primary types: low-density lipoprotein (LDL), often termed “bad cholesterol,” and high-density lipoprotein (HDL), known as “good cholesterol.” While HDL works to remove cholesterol from the bloodstream, LDL contributes to plaque buildup in arteries, leading to serious health risks. Among the organs affected by high levels of bad cholesterol, the heart and blood vessels bear the brunt of the damage.
The Heart and Blood Vessels: Primary Targets of LDL Cholesterol
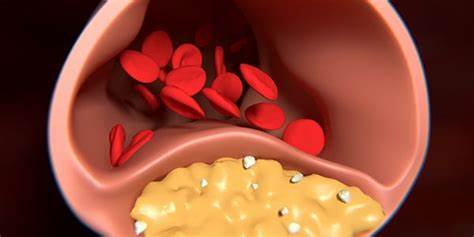
Bad cholesterol primarily affects the cardiovascular system. When LDL cholesterol levels are too high, it deposits on the walls of arteries, forming plaques in a process known as atherosclerosis. This condition narrows the arteries, restricting blood flow and increasing the risk of cardiovascular diseases, such as:
- Coronary Artery Disease (CAD): The buildup of plaque in the coronary arteries can lead to chest pain (angina) or even a heart attack.
- Peripheral Artery Disease (PAD): Plaque accumulation in the arteries supplying the limbs can cause pain, weakness, and restricted movement.
- Stroke: If plaques rupture, they can form clots that travel to the brain, causing a stroke.
- Hypertension: Narrowed arteries make it harder for the heart to pump blood, resulting in high blood pressure.
The Liver’s Role in Cholesterol Management
The liver plays a critical role in cholesterol regulation. It produces cholesterol naturally and helps remove excess LDL from the bloodstream by processing it into bile, which is excreted through the digestive system. However, when LDL levels rise, the liver may become overwhelmed, contributing to systemic issues.
Other Organs at Risk
While the cardiovascular system is the most affected, other organs are not spared from the harmful effects of bad cholesterol:
- Kidneys: Narrowed blood vessels reduce blood flow to the kidneys, impairing their ability to filter waste efficiently, potentially leading to chronic kidney disease.
- Brain: High cholesterol levels can increase the risk of vascular dementia and cognitive decline due to restricted blood flow to the brain.
- Eyes: LDL cholesterol can cause the development of yellowish deposits around the eyes (xanthelasma) and increase the risk of retinal artery occlusion.
- Pancreas: Cholesterol can contribute to inflammation in the pancreas, worsening conditions like pancreatitis and increasing the risk of diabetes.
Symptoms of High LDL Cholesterol
High LDL cholesterol often has no clear symptoms, earning it the nickname “silent killer.” However, advanced cases may present with:
- Chest pain or discomfort
- Fatigue and shortness of breath
- Leg pain or cramps while walking
- Yellowish patches around the eyes
- Elevated blood pressure
Because it’s largely asymptomatic in its early stages, regular cholesterol screening is essential.
Risk Factors for High LDL Cholesterol
Several factors contribute to elevated bad cholesterol levels, including:
- Dietary Choices: Consuming foods high in saturated fats and trans fats (e.g., fried foods, processed snacks, and red meats) significantly increases LDL levels.
- Lack of Physical Activity: Sedentary lifestyles lower HDL (good cholesterol), leaving LDL unchecked.
- Genetics: Familial hypercholesterolemia is a genetic condition leading to abnormally high cholesterol levels from birth.
- Smoking: Cigarettes damage blood vessels and reduce HDL levels, further complicating cholesterol management.
- Obesity: Excess body fat can lead to metabolic syndrome, contributing to high LDL cholesterol.
- Age and Gender: Cholesterol levels tend to rise with age, and postmenopausal women are at higher risk due to hormonal changes.
How to Lower Bad Cholesterol Levels
The good news is that bad cholesterol levels can be effectively managed through lifestyle changes and, if necessary, medications. Here are practical strategies to reduce LDL cholesterol:
1. Adopt a Heart-Healthy Diet
- Limit Saturated Fats: Reduce consumption of full-fat dairy products, red meat, and processed foods.
- Avoid Trans Fats: Check food labels for “partially hydrogenated oils,” commonly found in baked goods and margarine.
- Increase Fiber Intake: Soluble fiber, found in oats, beans, and fruits like apples and oranges, helps lower LDL levels.
- Choose Healthy Fats: Replace saturated fats with monounsaturated and polyunsaturated fats from sources like olive oil, avocados, and nuts.
- Incorporate Omega-3 Fatty Acids: Found in fatty fish like salmon, mackerel, and tuna, omega-3s improve overall heart health.
2. Stay Physically Active
- Aim for at least 30 minutes of moderate exercise five days a week. Activities like brisk walking, swimming, or cycling improve HDL levels and lower LDL cholesterol.
3. Quit Smoking
- Smoking cessation has immediate and long-term benefits for cholesterol management and overall cardiovascular health.
4. Limit Alcohol Intake
- While moderate alcohol consumption may increase HDL levels, excessive drinking contributes to high cholesterol and triglycerides.
5. Maintain a Healthy Weight
- Losing even a small amount of weight (5-10% of body weight) can significantly reduce LDL cholesterol levels.
Medical Treatments for High LDL Cholesterol
When lifestyle changes are insufficient, medical intervention may be necessary. Common treatments include:
- Statins: These drugs block a substance the liver needs to produce cholesterol, effectively lowering LDL levels.
- Ezetimibe: This medication reduces cholesterol absorption in the intestines.
- PCSK9 Inhibitors: These newer drugs help the liver absorb more LDL cholesterol from the bloodstream.
- Bile Acid Sequestrants: These drugs bind bile acids, forcing the liver to use excess cholesterol to produce more bile.
Natural Remedies to Lower LDL Cholesterol
For those seeking alternative approaches, certain natural remedies may help manage cholesterol levels:
- Garlic: Regular consumption of garlic may modestly reduce LDL levels.
- Green Tea: Rich in catechins, green tea helps lower LDL and improve overall heart health.
- Psyllium Husk: This soluble fiber supplement can help reduce cholesterol when consumed daily.
- Fenugreek Seeds: These seeds are rich in soluble fiber, aiding in cholesterol reduction.
The Importance of Regular Monitoring
To keep cholesterol levels in check, it’s crucial to undergo routine health checkups. A lipid profile test measures LDL, HDL, and total cholesterol levels, providing a clear picture of your cardiovascular risk. For individuals over 20, cholesterol testing is recommended every 4-6 years. Those with risk factors like obesity or a family history of heart disease should test more frequently.
Conclusion: Take Charge of Your Cholesterol Levels
Bad cholesterol poses a significant threat to the heart, blood vessels, and other vital organs. However, through mindful dietary choices, regular exercise, and, if needed, medical treatment, LDL levels can be effectively managed. Remember, prevention is always better than cure. By adopting a heart-healthy lifestyle and staying proactive about your health, you can protect your organs, improve your quality of life, and reduce your risk of life-threatening conditions. Take the first step today, because every small change counts in the journey to better health.