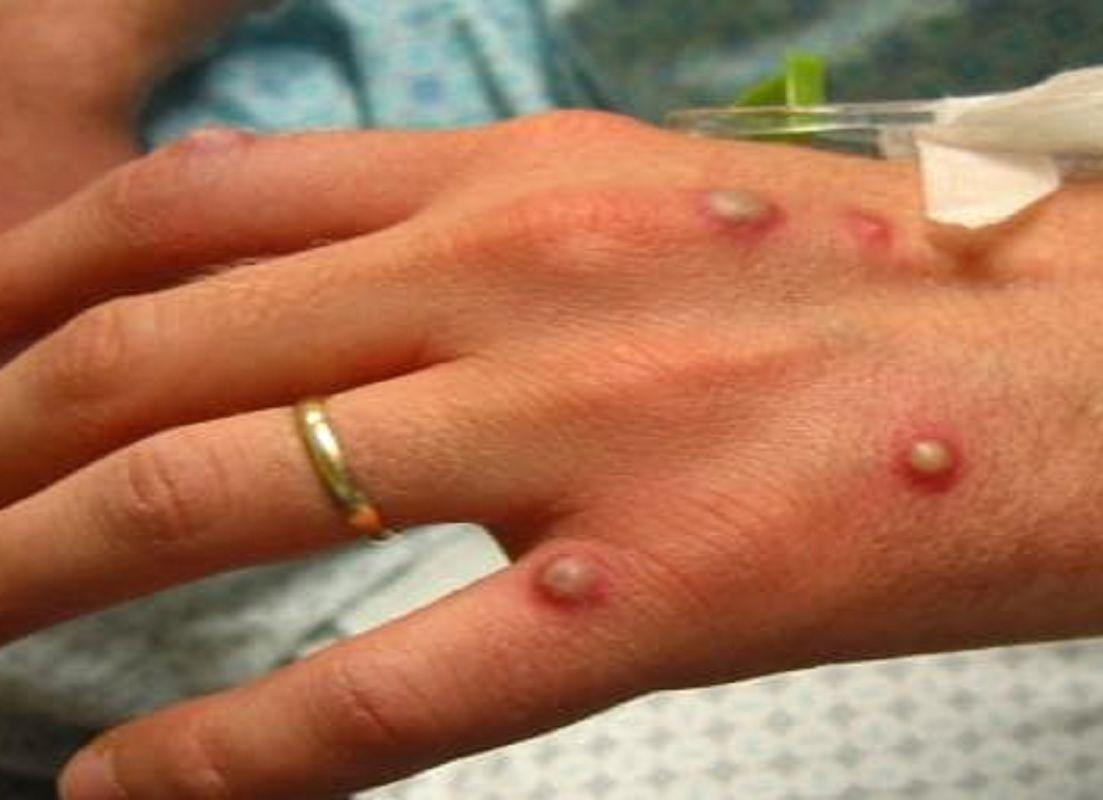
According to a research published on Saturday in The Lancet Infectious Diseases journal, the symptoms of monkeypox patients in the UK differ from those seen in past outbreaks throughout the world. The study included 54 people who visited sexual health clinics in London, UK, and were diagnosed with monkeypox over a 12-day period in May of this year.
The findings show that patients in this group had a greater incidence of vaginal and anal skin lesions and a lower prevalence of fatigue and fever than cases from previously investigated monkeypox outbreaks.
Based on these data, the researchers propose that current case criteria for ‘possible cases’ of monkeypox be revisited to aid in case identification.
They also expect that due to the high prevalence of genital skin lesions in patients, as well as the high rate of co-occurring sexually transmitted illnesses, sexual health clinics will encounter more monkeypox cases in the future. The researchers advocate for more resources to help services manage this illness.
“The UK and numerous other countries are currently experiencing a significant spike in monkeypox cases among persons attending sexual health clinics, with no clear ties to places where the illness is endemic,” said Nicolo Girometti of the Chelsea & Westminster Hospital NHS Foundation Trust.
“Monkeypox is a unique diagnosis in the sexual health field,” Girometti said. “Our study, the first to publish on cases from this UK epidemic, will benefit in future case detection and therapeutic management.” The researchers gathered information from monkeypox patients at four sexual health clinics in London, England. Individuals with laboratory-confirmed infection utilising an RT-PCR test were considered confirmed cases.
They took notes on the patient’s travel history, sexual history, and clinical complaints. Individuals diagnosed with monkeypox were instructed to isolate themselves and were then monitored on a regular basis via phone welfare checks. The 54 individuals examined in this study account for 60% of the cases reported in the United Kingdom over the 12-day study period in May of this year.
Except for two patients in the group, none had been in touch with a known case, and none had been to Sub-Saharan Africa, but several had recently visited other European nations. According to the study, all patients classified as males who had intercourse with men, with a median age of 41.
As many as 90% of patients who replied to the sexual activity questions reported at least one new sexual partner in the three weeks preceding symptoms, and virtually all reported inconsistent condom usage during this same time period.
According to the researchers, more than half of the patients had more than five sexual partners in the 12 weeks before their monkeypox diagnosis.
All of the patients were symptomatic and had skin lesions; 94% of the patients had at least one skin lesion on the vaginal or perianal area.
The majority of the patients had a moderate sickness and healed at home, but five required hospitalisation owing to discomfort or infection of the skin sores. All of them improved and were discharged after a median of seven days in the hospital.
“The commonly observed symptom of skin lesions in the anal and penile areas, as well as the fact that a quarter of the patients tested positive for gonorrhoea or chlamydia at the same time as the monkeypox infection, suggests that transmission of the monkeypox virus in this cohort occurs from close skin-to-skin, such as in the context of sexual activity,” said Ruth Byrne of the Chelsea & Westminster Hospital NHS Foundation Trust.
The clinical parameters of this cohort differed significantly from prior cases reported from past outbreaks in other countries, according to the researchers. According to the researchers, a lower number of patients in the group reported feeling weak and exhausted or having a fever than in prior outbreak investigations.
Furthermore, 18% of patients in the group did not report any early symptoms prior to the emergence of skin lesions, the researchers said.